Eating should be simple, but for many people living with Parkinson’s disease, tremor can turn mealtimes into a daily challenge. Learning how to reduce hand shaking during meals in Parkinson’s disease is not about control or perfection—it’s about using the right strategies to make eating easier and less stressful. From posture and pacing to food choices and support, small adjustments can make a meaningful difference. In this guide, you’ll discover practical ways to feel more confident and comfortable at the table.

Eating should be one of life’s simple pleasures, yet for many people with Parkinson’s disease, hand shaking can turn meals into a source of frustration or embarrassment. Learning how to reduce hand shaking during meals in Parkinson’s disease isn’t about eating “perfectly” — it’s about finding practical strategies that make meals calmer, safer, and more enjoyable.
This article provides a practical, Parkinson’s-specific guide to reducing hand shaking during meals. Rather than focusing on strength or control alone, it explains how posture, pacing, support, and everyday adjustments can make eating easier and more comfortable.
In this guide, you’ll learn:
- Why hand shaking often become worse during meals in Parkinson’s disease
- How body position and movement speed affect tremor
- Simple eating strategies that reduce shaking without strain
- Which adaptive tools and food choices are most helpful
- How medication timing and stress can influence hand control
The goal is not perfect eating, but calmer, more confident meals that support independence and enjoyment.
Why hand shaking gets worse during meals
For many people living with Parkinson’s disease, hand shaking is not constant — it often becomes more noticeable during specific tasks. Eating is one of the most common examples. Understanding why tremor worsens during meals is the first step toward managing it more effectively.
One reason is that eating requires precise, goal-directed movement. Bringing food from a plate to the mouth demands fine motor control, timing, and coordination between the hand, arm, and trunk. In Parkinson’s disease, these controlled movements place higher demands on motor circuits that are already under strain, making tremor more likely to appear or intensify.
Stress and attention also play a major role. Mealtimes — especially when eating with others — can create pressure to move quickly, avoid spills, or “eat normally.” This sense of urgency increases muscle tension and sympathetic nervous system activity, both of which can amplify hand shaking.
Fatigue is another contributing factor. Tremor often worsens later in the day or when the body is tired. If meals coincide with medication wearing off or general fatigue, hand control may feel less reliable.
Importantly, tremor during meals does not mean you are losing strength or control permanently. It reflects how Parkinson’s affects movement under demand. With the right strategies, many people can significantly reduce hand shaking during meals and feel more comfortable eating again.
In the next section, we’ll start with one of the most effective — and often overlooked — approaches: adjusting your body position before changing what or how you eat.
Adjust your body before you adjust the food

One of the most effective ways to reduce hand shaking during meals in Parkinson’s disease has nothing to do with utensils or food choices. It starts with how your body is positioned before the first bite.
Tremor often increases when the arms and hands are forced to work without adequate support. Sitting too far from the table, leaning forward, or holding the arms up against gravity all increase muscular effort and instability. In Parkinson’s disease, this extra effort can quickly amplify hand shaking.
Begin by focusing on a stable, supported posture. Sit upright with your back supported and both feet flat on the floor. Your hips and knees should be at a comfortable height, allowing you to sit without strain. When possible, rest your forearms lightly on the table or armrests. This support reduces the need for constant muscle activation and often leads to noticeably steadier hand movement.
Chair and table height also matter. If the table is too high, the shoulders lift, and tension builds in the arms. If it’s too low, you may lean forward, increasing tremor and fatigue. Small adjustments — such as adding a cushion to the chair or lowering the plate slightly — can make a meaningful difference.
Before lifting food, pause briefly. Take a slow breath and allow your shoulders and hands to relax. This moment of stillness helps reset muscle tension and reduces the urge to rush, which is a common trigger for shaking.
These changes may seem minor, but they directly address how Parkinson’s affects movement under load. Many people notice that once their body feels stable and supported, hand shaking during meals becomes easier to manage — even before introducing tools or other strategies.
In the next section, we’ll look at simple eating techniques that further reduce tremor by slowing movement and increasing control.
Simple eating strategies that reduce shaking
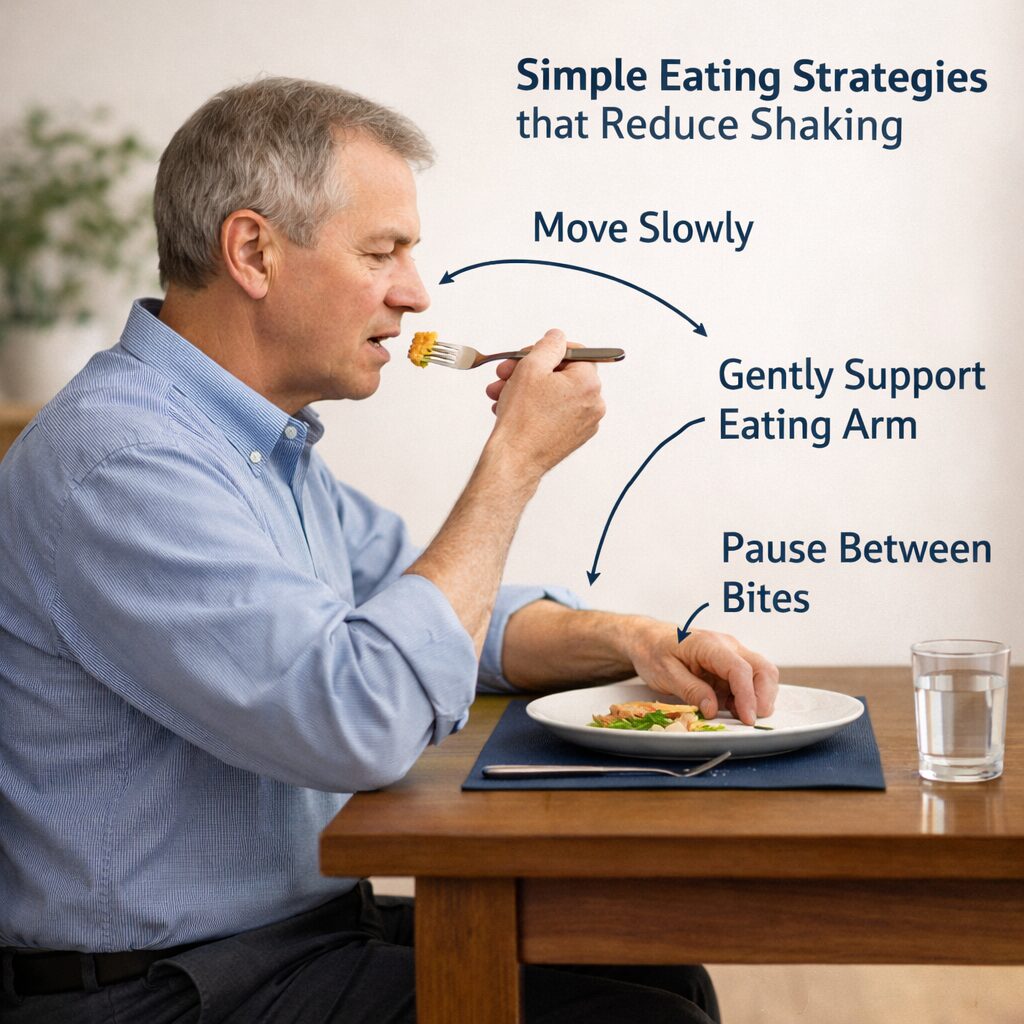
Once your body is supported and settled, how you move during meals becomes just as important as what you eat. In Parkinson’s disease, tremor often increases with speed, urgency, and overcorrection — all of which are common during eating.
One of the most effective strategies is to slow the entire eating sequence. Instead of lifting food quickly from plate to mouth, move in a smooth, deliberate arc. Slower movement gives the nervous system more time to coordinate the action and often reduces shaking mid-movement.
Stabilizing the arm can also help. Lightly resting the elbow or forearm on the table while lifting food decreases the effort required to control the hand. Some people find it helpful to use the non-eating hand to gently support the wrist or forearm of the eating hand, especially during the final movement toward the mouth.
Pausing between bites is another powerful but underused technique. After each bite, place the utensil down, relax your hands, and take a breath. This brief reset prevents tremor from building with repeated movements and reduces overall fatigue during the meal.
Grip pressure matters as well. Overgripping utensils increases muscle tension and makes tremor more pronounced. Aim for a relaxed, functional grip rather than a tight one. If you notice your hand tensing, consciously loosen your fingers before the next bite.
Finally, pay attention to breathing. Holding your breath — which often happens unconsciously when concentrating — can worsen shaking. Steady, natural breathing supports smoother movement and helps keep tremor from escalating.
These strategies may feel unfamiliar at first, especially if you’re used to trying to “push through” tremor. With practice, they become second nature and can significantly improve comfort and confidence at mealtimes.
In the next section, we’ll explore adaptive tools that can provide additional support — and explain when they help most, and when they don’t.
Adaptive tools that actually help

Adaptive eating tools are often recommended for Parkinson’s disease, but their usefulness varies from person to person. The goal of these tools is not to eliminate tremor, but to reduce the effort required to manage it, making meals less tiring and more predictable.
One of the most commonly used options is weighted utensils. For some people, the added weight helps dampen hand shaking by increasing sensory feedback and slowing movement. Weighted utensils tend to work best for mild to moderate action tremor and when fatigue is a major contributor. However, they are not universally helpful. For people with significant rigidity, weakness, or shoulder fatigue, extra weight can actually worsen control. It’s worth trying them briefly before committing to regular use.
Built-up handles are often more broadly useful. Thicker handles reduce the need for tight gripping, which in turn lowers muscle tension in the hand and forearm. This can make tremor less noticeable and improve endurance during meals. Built-up handles are especially helpful if finger stiffness or cramping accompanies tremor.
Plate guards and bowls with higher sides can also reduce shaking-related spills. By limiting how far food can slide, they reduce the precision required for scooping. This allows the hand to move more confidently and with less correction, which often reduces tremor during the task.
Cups with lids or straws can help manage liquids, which are often harder than solid foods when hand shaking is present. These tools reduce the need for fine control and help prevent spills that increase frustration and self-consciousness.
It’s important to remember that tools are supports, not solutions. They work best when combined with good posture, slower movement, and reduced pressure. If a tool feels awkward, heavy, or frustrating, it’s okay to set it aside. The “best” tool is the one that makes eating feel easier, not more complicated.
In the next section, we’ll look at how food choices and meal modifications can further reduce hand shaking and make eating more manageable.
Food and meal modifications that make eating easier

What you eat and how food is prepared can have a significant impact on how much hand shaking interferes with meals in Parkinson’s disease. The goal is not to restrict enjoyment, but to reduce unnecessary precision demands when tremor is most active.
Food texture plays an important role. Foods that are very small, slippery, or require cutting on the plate tend to increase shaking because they demand fine motor control and repeated corrections. Softer foods, cohesive textures, and items that stay together on a fork or spoon are generally easier to manage when tremor is present.
Cutting food into smaller, ready-to-eat pieces before sitting down can make a surprising difference. This reduces the need for two-handed coordination and limits the time spent manipulating food on the plate, when tremor often becomes more noticeable.
Using finger foods strategically is another practical option. Eating with the hands is not a failure or a step backward — it is often a more stable and efficient way to nourish yourself, especially on days when tremor is worse. Many nutritious foods can be adapted into finger-friendly forms without sacrificing dignity or enjoyment.
Liquids deserve special attention. Soups, thin sauces, and beverages are often the most challenging items during meals. Thicker liquids, smoothies, or foods with more body are usually easier to control. When possible, choosing foods that require fewer transitions between plate, utensil, and mouth reduces opportunities for shaking to escalate.
Meal timing also matters. Eating when you are already fatigued or rushed increases tremor. If possible, schedule meals during times of day when medication is working best and energy is higher. Smaller, more frequent meals may also be easier to manage than large ones that require sustained effort.
These adjustments are not about limitation — they are about reducing effort so your hands can do less work. When food choices support steadier movement, many people find meals become calmer and more enjoyable again.
In the next section, we’ll look at how medication timing and symptom fluctuations interact with hand shaking during meals — and when it’s worth discussing changes with your care team.
Medication timing and meals

Hand shaking during meals often fluctuates with medication cycles in Parkinson’s disease. Tremor may worsen when the medication is wearing off or before the next dose has fully taken effect. If meals regularly fall during these low-response periods, eating can feel significantly harder than at other times of day.
When possible, scheduling meals during your best “ON” periods can make a noticeable difference. This doesn’t mean delaying food excessively, but small timing adjustments — such as eating slightly later or earlier — may reduce tremor and improve control. Light movement before meals can also help medication absorption for some people.
If hand shaking during meals has changed suddenly or become much more disruptive, it’s worth discussing this with your clinician. Medication adjustments won’t eliminate tremor completely, but optimizing timing can often reduce how much it interferes with daily activities like eating.
Next, we’ll look at an often-overlooked factor: the emotional and social stress around meals, and how reducing pressure can calm tremor more than trying harder ever will.
Managing social and emotional stress at mealtimes

Hand shaking during meals is not only a physical issue — it is strongly influenced by stress, attention, and self-consciousness. In Parkinson’s disease, anxiety and urgency can amplify tremor even when physical control hasn’t changed. This is why shaking often feels worse when eating with others or in public settings.
Reducing pressure can make a real difference. Eating more slowly, choosing quieter environments, or starting meals alone before joining others can help calm the nervous system. Letting trusted companions know that tremor may vary removes the need to “perform” or hide symptoms, which often reduces shaking on its own.
Reframing expectations is equally important. Meals do not need to look neat or fast to be successful. Focusing on nourishment, comfort, and enjoyment — rather than appearance — helps shift attention away from the tremor itself. This mental shift often leads to steadier movement than trying to control the shaking directly.
Practical takeaway for patients
Hand shaking during meals is a common and frustrating part of Parkinson’s disease, but it is often modifiable. Small changes in posture, pacing, support, and food choices can significantly reduce how much tremor interferes with eating.
The most effective approach is not trying harder, but making eating easier. Supporting the arms, slowing movements, choosing forgiving foods, and reducing pressure at mealtimes all help calm the nervous system and improve control.
Above all, remember that eating is about nourishment and comfort — not precision or appearance. When meals are approached with patience rather than urgency, many people find they regain confidence and enjoyment at the table.
Disclaimer: The information shared here should not be taken as medical advice. The opinions presented here are not intended to treat any health conditions. For your specific medical problem, consult with your healthcare provider.
Track your Parkinson’s day in less than a minute
The Parkinson’s Daily Diary App lets you record symptoms, medications, daily notes and doctor ready report in under a minute.
