Medication can dramatically improve symptoms in Parkinson’s disease — but only when timing works with the brain, not against it. Many Parkinson’s patients take the right pills but still struggle with stiffness, tremor, or sudden OFF periods because when medication is taken matters just as much as what is taken. Understanding Parkinson’s pill timing can help smooth symptom fluctuations, reduce wearing-off, and make daily life more predictable.

For many people living with Parkinson’s disease, medication is a lifeline — yet symptoms can still fluctuate unpredictably throughout the day. Tremor may return before the next dose, stiffness may appear suddenly, or mornings may feel especially difficult despite taking the “right” pills. In many cases, these challenges are not about medication choice, but about timing.
Understanding how and when Parkinson’s medications work and why timing matters so much can help reduce OFF periods, smooth symptom control, and make daily life feel more predictable.
This article is a practical, easy-to-follow guide to Parkinson’s pill timing, written for patients and caregivers.
In this guide, you’ll learn:
- Why Parkinson’s pill timing matters
- How medication timing affects ON and OFF periods
- Common timing mistakes that worsen symptoms
- How meals, protein, and digestion influence medication absorption
- Practical strategies to build a pill schedule that actually works
- When timing issues should be discussed with your clinician
The goal is not perfect control, but more consistent days with fewer surprises — using timing as a tool rather than a source of stress.
Why Parkinson’s pill timing matters
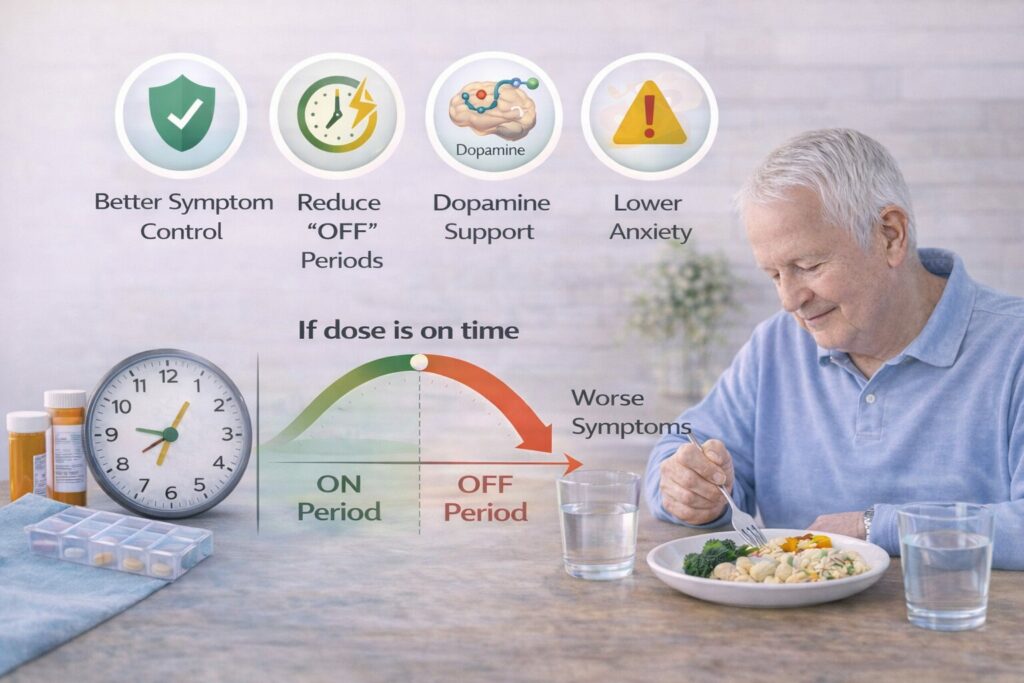
In Parkinson’s disease, medication timing is not a minor detail — it is a central part of treatment. Many people take the correct medication at the correct dose and still experience stiffness, tremor, slowness, or sudden OFF periods simply because the timing does not match how their body absorbs and uses the medication.
Parkinson’s medications, especially those that replace or support dopamine, work within relatively short and variable time windows. Unlike medications that provide steady coverage over many hours, Parkinson’s pills often rise and fall in effect. This means that taking a dose even 30–60 minutes later than usual can noticeably change how someone feels and moves.
Another reason timing matters is that Parkinson’s disease symptoms are not static. They fluctuate throughout the day based on medication levels, fatigue, stress, digestion, and activity. When pill timing is inconsistent, these natural fluctuations can become more pronounced, leading people to feel as though the disease itself is rapidly worsening — when in fact, the issue may be wearing-off rather than progression.
Timing also affects predictability. When doses are taken at consistent intervals, the brain learns to expect dopamine support, and symptom control becomes more reliable. When timing varies from day to day, ON and OFF periods become harder to anticipate, increasing anxiety and reducing confidence in daily planning.
Importantly, pill timing is not about perfection. It is about alignment — aligning medication intake with how the Parkinson’s brain functions, how the gut absorbs medication, and how symptoms tend to fluctuate. Learning to respect timing can often smooth symptoms without changing the medication itself.
In the next section, we’ll look at how Parkinson’s disease medications actually work in the body, and why absorption, digestion, and delivery to the brain are just as important as the pill you take
How Parkinson’s disease medications work in the body
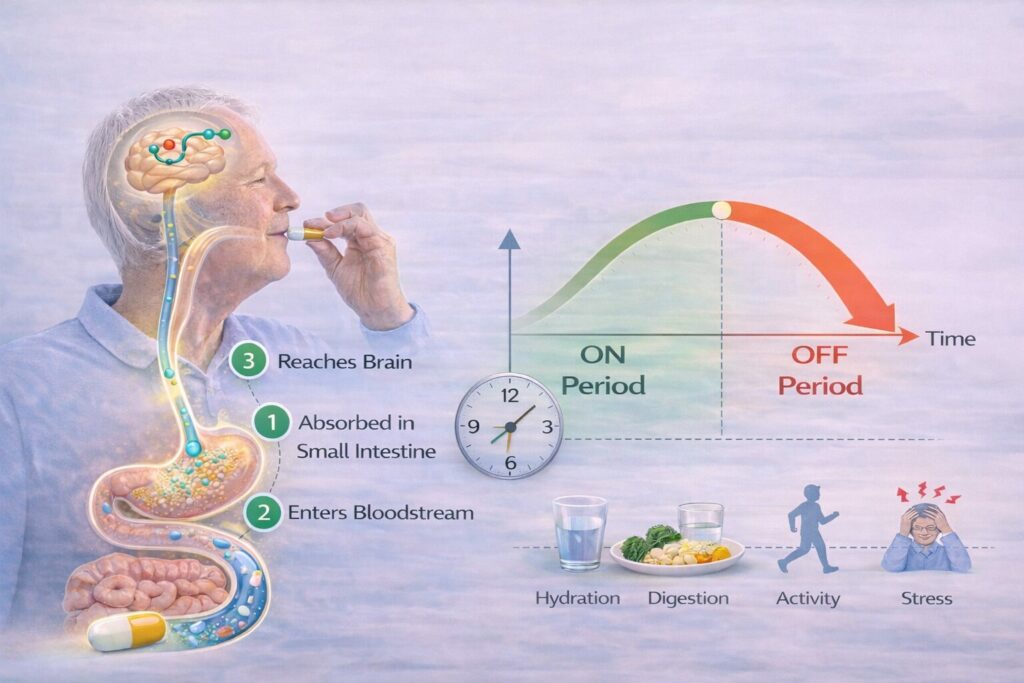
To understand Parkinson’s pill timing, it helps to know what happens after you swallow a pill. In Parkinson’s disease, most medications aim to replace or support dopamine — a chemical the brain uses to control movement. Because dopamine itself cannot cross into the brain, treatment relies on medications that must be absorbed, transported, and converted before they can help.
For many people, this process is not instant and not consistent. After swallowing a pill, it must first pass through the stomach and into the small intestine, where absorption occurs. From there, it enters the bloodstream and eventually reaches the brain. Any delay along this path — slow stomach emptying, constipation, or competition with food — can delay or weaken the medication’s effect.
This is why the same dose can feel different on different days. Factors such as hydration, stress, physical activity, and especially digestion influence how quickly medication starts working. In Parkinson’s disease, gastrointestinal motility is often slower, which means medication absorption can be unpredictable even when pills are taken correctly.
Once medication reaches the brain, its effect does not last indefinitely. Dopamine support rises, reaches a peak, and then gradually falls. As Parkinson’s disease progresses, the brain becomes less able to buffer these changes, making timing more important. The result is shorter ON periods and more noticeable OFF periods if doses are delayed or inconsistent.
Understanding this process helps explain why timing matters so much. It’s not just about taking pills — it’s about helping the medication arrive when the brain needs it most.
In the next section, we’ll look more closely at ON periods, OFF periods, and wearing-off, and how timing errors can make these fluctuations feel more severe than they need to be.
ON periods, OFF periods, and wearing-off
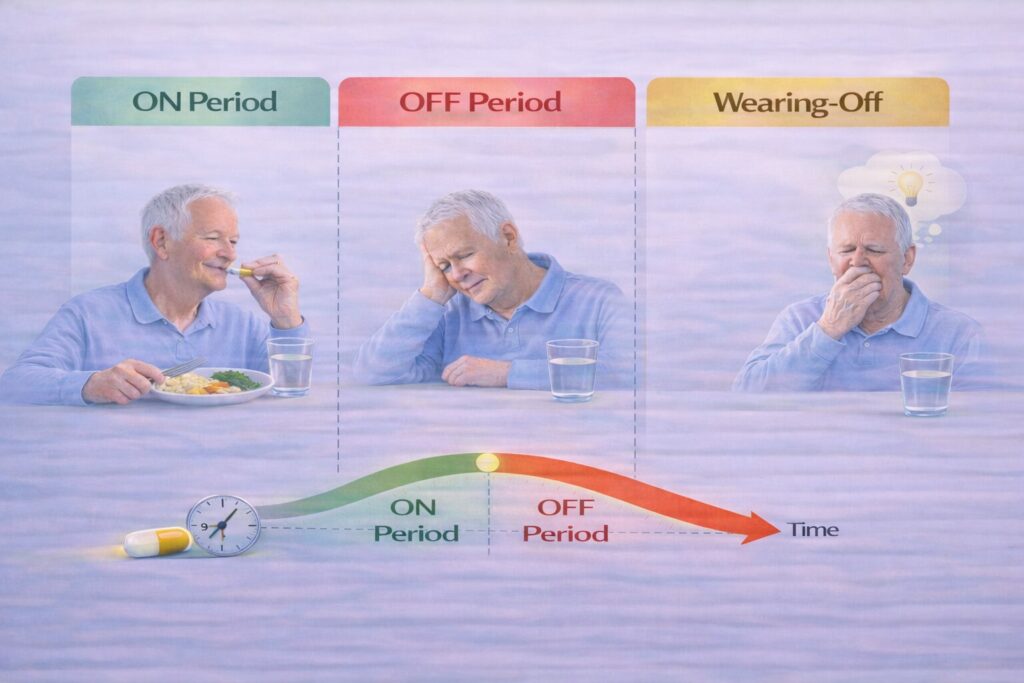
People living with Parkinson’s disease often describe their day in terms of ON and OFF time. Understanding these states is essential for making sense of pill timing — and for recognizing when timing, rather than disease progression, is the main issue.
An ON period is when medication is working well. Movement feels smoother, stiffness eases, and daily tasks are easier. An OFF period occurs when medication effects fade, leading to the return of symptoms such as slowness, rigidity, tremor, anxiety, or difficulty walking. These shifts can happen gradually or quite suddenly.
Wearing-off refers to the predictable return of symptoms before the next scheduled dose. Early signs are often subtle and easy to miss: increased fatigue, softer voice, slowed thinking, mild anxiety, or a sense that tasks take more effort. Because these changes don’t always look dramatic, many people assume they’re part of normal fluctuation — or that Parkinson’s disease is worsening — when the real issue is timing.
Timing errors can amplify wearing-off. Taking doses late, spacing them unevenly, or delaying medication until symptoms feel severe often shortens ON time and deepens OFF periods. Over time, this pattern can make days feel unpredictable and exhausting, even when the medication itself is still effective.
Recognizing ON, OFF, and wearing-off patterns is empowering. It allows patients and caregivers to see timing as a modifiable factor. In many cases, adjusting when medication is taken — without changing the dose — can smooth fluctuations and restore a sense of control.
In the next section, we’ll look at common pill-timing mistakes and why they unintentionally make symptoms harder to manage.
Common pill-timing mistakes (and why they matter)
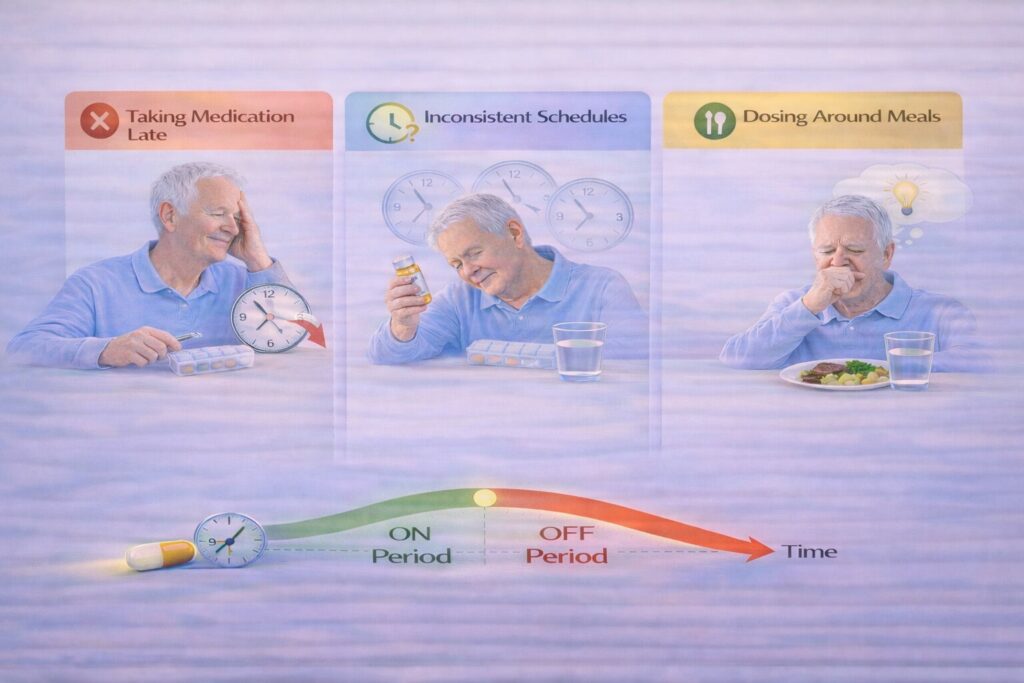
Many challenges with Parkinson’s disease pill timing are not caused by the medication itself, but by a few common — and very understandable — timing habits. Recognizing these patterns can make a meaningful difference in daily symptom control.
One frequent mistake is taking medication late and waiting until symptoms feel uncomfortable before dosing. While this may seem logical, it often allows dopamine levels to drop too far, making it harder for the next dose to fully restore movement. Over time, this can deepen OFF periods and shorten ON time.
Another issue is inconsistent scheduling. Taking the same medication at different times each day — even by an hour — can lead to unpredictable symptom control. Parkinson’s disease medications work best when the brain can anticipate regular dopamine support. Irregular timing disrupts that rhythm and increases fluctuations.
Some people also space doses too closely together to chase symptom relief, which can increase side effects without improving control. Others skip or delay doses around meals without realizing how food, especially protein, can affect absorption.
These mistakes are common because Parkinson’s pill timing is rarely explained clearly. The good news is that most timing issues are fixable with awareness and small adjustments.
In the next section, we’ll focus on how food, protein, and digestion interact with Parkinson’s disease medications, and what timing strategies actually help in real life.
Food, protein, and medication timing
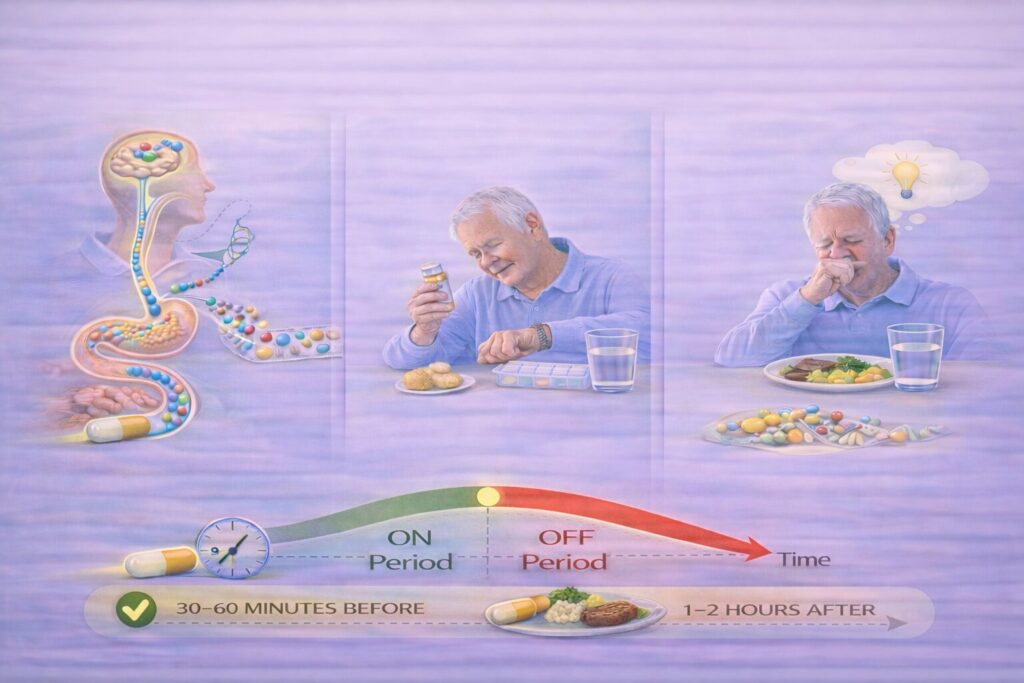
Food, especially protein, plays a major role in Parkinson’s disease pill timing, yet it’s one of the most confusing aspects for patients and caregivers. This is because some Parkinson’s disease medications, particularly those based on levodopa, use the same transport pathways in the gut and brain as dietary amino acids. When large amounts of protein are present at the same time, medication absorption and delivery can be reduced or delayed.
This interaction does not mean protein should be avoided. Protein is essential for health, strength, and energy. The key is timing, not restriction. Many people find that taking medication 30–60 minutes before meals, or 1–2 hours after eating, allows it to work more reliably. Others benefit from shifting most protein intake to later in the day, when motor demands are lower.
Digestion also matters. Parkinson’s disease commonly slows stomach emptying and bowel motility, which can delay when medication reaches the intestine for absorption. Constipation, dehydration, and large meals can all contribute to unpredictable response. Staying well hydrated, eating smaller meals, and maintaining regular bowel habits can indirectly improve medication timing effectiveness.
Importantly, not everyone is equally sensitive to food–medication interactions. The goal is not rigid rules, but pattern awareness. If symptoms consistently worsen after meals or improve when medication is taken on an empty stomach, timing adjustments may help.
In the next section, we’ll look at how to build a medication schedule that fits real life, rather than forcing life to fit the pills.
Building a Parkinson’s disease medication schedule that actually works

A medication schedule that helps in Parkinson’s disease is one that fits real life — not one that feels rigid or overwhelming. The goal of Parkinson’s pill timing is consistency with flexibility, allowing medication to support daily activities as reliably as possible.
Start by anchoring doses to time, not symptoms. Taking medication at regular, planned intervals helps maintain steadier dopamine levels and reduces sudden OFF periods. Using alarms, phone reminders, or pill timers can remove the mental burden of remembering doses and reduce accidental delays.
It’s also helpful to observe your own patterns. Keep a simple log for a few days noting when medication is taken, when symptoms improve, and when they return. This can reveal predictable wearing-off patterns and help guide small timing adjustments — often without changing the dose itself.
Flexibility matters because days are not identical. Travel, appointments, and sleep changes can disrupt schedules. When this happens, aim to protect dose spacing rather than exact clock times. Small shifts are usually better than skipping or stacking doses.
Most importantly, medication schedules should be reviewed and adjusted with your clinician, especially if OFF periods are frequent or severe. Pill timing is a skill that improves with practice and guidance. When timing works, many people experience smoother days and greater confidence managing Parkinson’s disease symptoms.
In the next section, we’ll look at special situations — such as morning OFF, nighttime symptoms, and travel — where pill timing often needs extra attention.
Special situations where pill timing needs extra attention

Even with a well-planned schedule, there are situations where Parkinson’s pill timing becomes more challenging. Recognizing these scenarios helps prevent frustration and unnecessary symptom escalation.
Morning OFF is one of the most common issues. After hours without medication, stiffness, slowness, or tremor may be pronounced on waking. Some people benefit from taking their first dose immediately upon waking, while others use clinician-approved strategies such as fast-acting formulations or timing adjustments to shorten this OFF period. Gentle movement and hydration can also support medication onset.
Evening wearing-off is another frequent pattern. As the day progresses, medication effects may shorten, leading to increased symptoms late in the afternoon or evening. Adjusting dose timing earlier — rather than adding extra doses — sometimes smooths this transition. Noting when symptoms reliably return helps guide these changes.
Nighttime symptoms such as rigidity, difficulty turning in bed, or early-morning awakening may signal that medication coverage is insufficient overnight. These issues should always be discussed with a clinician, as nighttime dosing strategies differ from daytime ones.
Travel and schedule changes can disrupt even the best routine. When crossing time zones or facing long days, prioritize keeping dose intervals consistent rather than matching exact clock times. Planning ahead and setting alarms reduces missed or delayed doses.
These situations don’t mean your schedule is failing — they highlight where timing needs refinement.
In the next section, we’ll focus on what caregivers should know about pill timing, and how they can support consistency without adding pressure.
What caregivers should know about Parkinson’s pill timing

Caregivers often play a central role in managing Parkinson’s pill timing, especially as symptoms fluctuate or routines become more complex. Understanding a few key principles can help caregivers provide effective support without turning medication into a constant source of stress.
One of the most important roles caregivers can play is pattern observation. Noticing when symptoms reliably improve after a dose, when they begin to wear off, or when medication seems delayed can provide valuable information for timing adjustments. Sharing these observations with the care team often leads to more effective changes than simply reporting “good” or “bad” days.
Consistency is another area where caregivers make a difference. Helping maintain regular dose intervals, setting reminders, or preparing pill organizers reduces missed or delayed doses. At the same time, flexibility is essential — supporting small timing shifts when needed rather than insisting on rigid schedules.
Caregivers should also watch for non-motor signs of OFF periods, such as anxiety, fatigue, confusion, or mood changes. These symptoms are often overlooked but can signal wearing-off just as clearly as changes in movement.
Perhaps most importantly, pill timing should be a shared process. Involving the person with Parkinson’s disease in decisions preserves autonomy and reduces frustration. When caregivers act as partners rather than enforcers, medication timing becomes easier to manage for everyone.
In the final section, we’ll bring everything together with a practical takeaway for patients, focusing on confidence, not perfection.
Practical takeaway for patients
Managing Parkinson’s pill timing is not about taking medication perfectly — it’s about learning how your body responds and using that knowledge to reduce unnecessary OFF time. Small, consistent timing adjustments often make a bigger difference than changing medications or increasing doses.
Pay attention to patterns rather than isolated moments. Notice when symptoms reliably improve, when they return, and how meals, stress, or fatigue affect medication response. These observations give you useful information and help guide productive conversations with your care team.
Most importantly, timing is a skill, not a test. It improves with awareness, routine, and support. When medication timing works with your daily life instead of fighting it, many people experience smoother days, fewer surprises, and greater confidence living with Parkinson’s disease.
Disclaimer: The information shared here should not be taken as medical advice. The opinions presented here are not intended to treat any health conditions. For your specific medical problem, consult with your healthcare provider.
Track your Parkinson’s day in less than a minute
The Parkinson’s Daily Diary App lets you record symptoms, medications, daily notes and doctor ready report in under a minute.
